Think back to the last time you injured yourself. Perhaps you fell over and hurt your knee, or sprained your ankle playing sport. Along with the pain, you can probably recall how swollen, red and hot the area became. These changes were a sign of your body’s protective inflammatory response springing into action. Although uncomfortable,
]]>Think back to the last time you injured yourself. Perhaps you fell over and hurt your knee, or sprained your ankle playing sport. Along with the pain, you can probably recall how swollen, red and hot the area became. These changes were a sign of your body’s protective inflammatory response springing into action.
Although uncomfortable, inflammation enabled you to heal by forcing you to rest the affected limb and avoid injuring yourself further; protecting the area from infection; and clearing away damaged tissue. As healing occurred, the swelling and redness resolved, and your ankle went back to normal.
If a sprained ankle is what you think of when you hear the word ‘inflammation’, you are probably wondering what a simple injury and depression could possibly have in common. The answer is, more than you think.
Burn, Baby, Burn
There is a type of inflammation you can’t see as it may not be localized to a particular area, or have an obvious trigger, such as an injury. Instead, it’s systemic (affecting multiple areas throughout the body), and occurs on a microscopic scale.
However, just like the inflammation of a sprained ankle, systemic inflammation begins as a protective response to a trigger, such as infection or cell damage, and is designed to help you heal. Unfortunately, if the trigger is persistent, as in the case of chronic disease or infection, environmental exposure to irritants (e.g. pollution, smoking), or even chronic stress, then the inflammation remains constant. This creates a chronic, low-grade inflammatory state, which may damage healthy tissue and disrupt the functioning of many body systems and organs – including your brain.

Sick, Tired, and Depressed
To understand how chronic inflammation can affect mood, let’s consider something called ‘sickness behaviour’. Think back to a time when you had a significant infection – perhaps it was influenza, or a bad bout of bronchitis. How did you feel?
If you’re like most people, you were exhausted; struggled to think; lost your appetite, your sense of pleasure, and your desire to spend time with others; and you probably felt very down. Rather than purely being caused by illness, these feelings were also a consequence of inflammation and, again, were designed to help you heal. How? By creating ‘sickness behaviours’, such as resting and keeping away from other people, which give you the best chance to recover without spreading the infection to others.
If you’re one of the 1.16 million Australians struggling with depression,1 you will have noticed the similarities between the feelings described above – such as a low mood, anhedonia (loss of pleasure) and fatigue – and how you feel when you’re depressed.
So, if inflammation can create depression-like feelings and behaviours in the context of being sick, can it cause depression in an otherwise healthy person?
Brain on Fire
Although inflammation and depression are definitely linked, researchers are still trying to establish which comes first, inflammation or depression. Here is what we know so far:
- Otherwise healthy people with depression have higher levels of markers of inflammation in their blood compared with non-depressed, healthy individuals, including the systemic inflammatory marker, C-reactive protein (CRP)2
- Children with elevated levels of CRP in their blood are more likely to develop depression 5 to 10 years later as young adults3
- People who have been depressed for a long time show 30% more brain inflammation than those who are depressed for a shorter amount of time4
- Depression is significantly more likely to develop in people with other inflammatory disorders, such as rheumatoid arthritis, chronic pain, obesity, diabetes, and cardiovascular disease5
- Anti-inflammatory medications have been shown to reduce the severity of symptoms of depression6
Grab the Fire Extinguisher
The good news is that reducing your level of inflammation (also called your ‘inflammatory load’) could help with your mood. You can influence your inflammatory load by tweaking your daily diet, exercise and supplements. Here are some tips to get you started
Anti-inflammatory foods
Your diet can either promote or reduce inflammation. In fact, people who end up developing depression often have higher intakes of pro-inflammatory foods such as sugar, unhealthy fats, and carbohydrates.7 Swap these foods for anti-inflammatory choices, such as fruits, vegetables, legumes, nuts, seeds, wholegrains and fatty fish. It can be as easy as starting with a bowl of lightly steamed vegetables, a tin of salmon, and some brown rice for lunch.

Exercise
Just 20 minutes of moderate exercise, such as brisk walking, dancing, gardening or gentle cycling, has been shown to significantly reduce inflammation.8 Additionally, exercise provides well-known mood-boosting benefits, such as an increase in endorphins (feel-good brain chemicals). Start with whatever you can commit to doing at least three times a week, and build from there.
Supplements
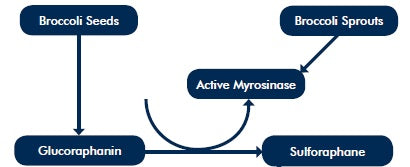
Turmeric is one of the most well-researched anti-inflammatory supplements. It significantly improves symptoms of depression when taken for at least four to six weeks, and also reduces anxiety in depressed people, without causing any unwanted side effects.9 In fact, a specific turmeric extract, known as BCM-95™, combined with saffron has shown similar benefits to an antidepressant medication.10

Put Out the Fire for a Better Mood
Inflammation and depression are inextricably linked. Regardless of which comes first, reducing your inflammatory load is vital in the fight against depression, enabling you to put out the fire of inflammation and achieve a healthy mood. For help changing your diet and exercise habits, or to help you choose the supplements that will be the best fit for you, get in touch with Kevin Tresize ND your natural healthcare Practitioner.
1 Australian Bureau of Statistics, National Survey of Mental Health and Wellbeing: Summary of Results [Internet]. Canberra ACT: Australian Bureau of Statistics 2007 [Accessed 27 November 2019] Available from: https://www.ausstats.abs.gov.au/ausstats/subscriber.nsf/0/6AE6DA447F985FC2CA2574EA00122BD6/$File/National%20Survey%20of%20Mental%20Health%20and%20Wellbeing%20Summary%20of%20Results.pdf.
2 Slavich GM, Irwin MR. From stress to inflammation and major depressive disorder: a social signal transduction theory of depression. Psychol Bull. 2014 May;140(3):774. doi: https://dx.doi.org/10.2105%2FAJPH.2014.302110.
3 Khandaker GM, Pearson RM, Zammit S, Lewis G, Jones PB. Association of serum interleukin 6 and C-reactive protein in childhood with depression and psychosis in young adult life: a population-based longitudinal study. JAMA Psychiatry. 2014 Oct 1;71(10):1121-8. doi: 10.1001/jamapsychiatry.2014.1332.
4 Setiawan E, Attwells S, Wilson AA, Mizrahi R, Rusjan PM, Miler L, et al. Association of translocator protein total distribution volume with duration of untreated major depressive disorder: a cross-sectional study. Lancet Psychiatry. 2018 Apr 1;5(4):339-47. doi: https://doi.org/10.1016/S2215-0366(18)30048-8.
5 Slavich GM, Irwin MR. From stress to inflammation and major depressive disorder: a social signal transduction theory of depression. Psychol Bull. 2014 May;140(3):774. doi: https://dx.doi.org/10.2105%2FAJPH.2014.302110.
6 Slavich GM, Irwin MR. From stress to inflammation and major depressive disorder: a social signal transduction theory of depression. Psychol Bull. 2014 May;140(3):774. doi: https://dx.doi.org/10.2105%2FAJPH.2014.302110.
7 Firth J, Veronese N, Cotter J, Shivappa N, Hebert J, Ee C, Smith L, Stubbs B, Jackson S, Sarris J. What is the role of dietary inflammation in severe mental illness? A review of observational and experimental findings. Front Psychiatry. 2019;10:350. doi: https://dx.doi.org/10.3389%2Ffpsyt.2019.00350.
8 Dimitrov S, Hulteng E, Hong S. Inflammation and exercise: Inhibition of monocytic intracellular TNF production by acute exercise via β2-adrenergic activation. Brain Behav Immun. 2017 Mar 1;61:60-8. doi: https://doi.org/10.1016/j.bbi.2016.12.017
9 Ng QX, Koh SS, Chan HW, Ho CY. Clinical use of curcumin in depression: A meta-analysis. Journal of the American Medical Directors Association. 2017 Jun 1;18(6):503-8. doi: https://doi.org/10.1016/j.jamda.2016.12.071.
10 Sanmukhani J, Satodia V, Trivedi J, Patel T, Tiwari D, Panchal B, Goel A, Tripathi CB. Efficacy and safety of curcumin in major depressive disorder: a randomized controlled trial. Phytother Res. 2014 Apr;28(4):579-85.
]]>